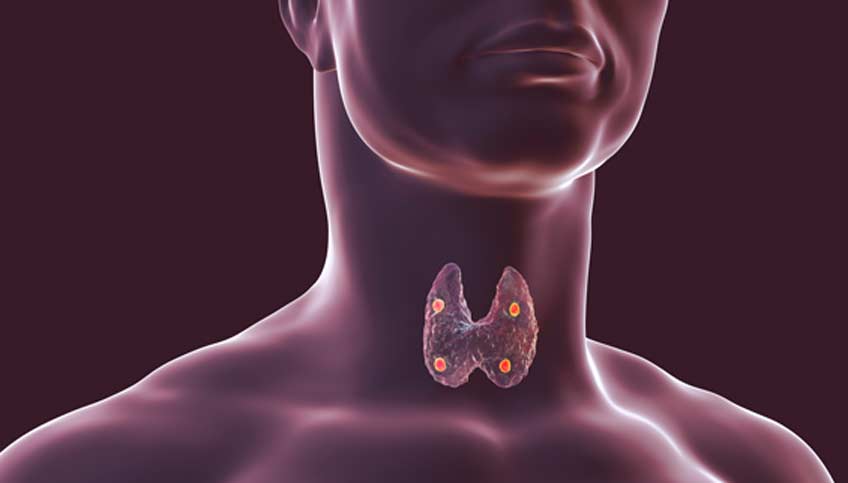
While it’s preferable to remove only a portion of this gland whenever possible, there are treatments that can make comfortably living without the entire thyroid gland possible.
If there is a need to remove all or part of the thyroid gland, the procedure that achieves this goal is known as a thyroidectomy. Found at the base of the neck, the butterfly-shaped thyroid gland plays a key role in various functions, including ones related to metabolism.
Why Is a Thyroidectomy Necessary?
A thyroidectomy is generally considered a last resort treatment. One reason for this procedure is a lack of response to medication for an overactive thyroid (hyperthyroidism). Thyroid removal may also be an option for patients not preferring radioactive iodine therapy. A more common reason for a thyroidectomy is thyroid cancer. A large goiter that’s causing breathing difficulties or problems with swallowing may also be a reason why partial or full thyroid removal is recommended.
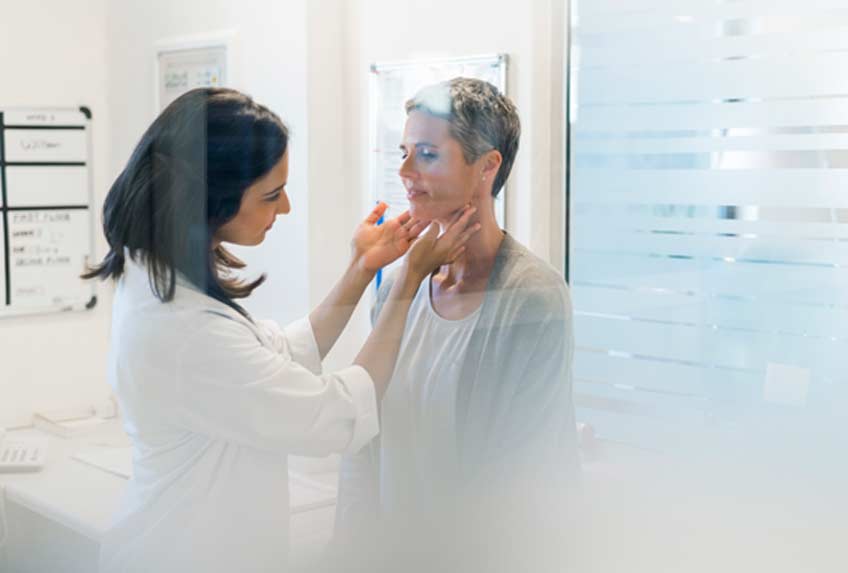
What Happens Before Surgery?
Medication that often includes an iodine and potassium solution may be recommended prior to surgery if the reason for thyroid removal is hyperthyroidism to reduce the risk of excessive bleeding. Additional precautions may be recommended to minimize issues with anesthesia complications prior to surgery.
How Is a Thyroidectomy Performed?
A traditional thyroidectomy is performed with a single incision that’s made in the center of the neck to access the thyroid gland. With an endoscopic thyroidectomy, smaller incisions are made in the neck to remove all or part of the thyroid gland. A lighted scope with a camera attached is inserted through one of the incisions to provide visual guidance. Specialized surgical instruments are also used so incisions can be kept small.
Another minimally invasive approach to thyroid removal is a robotic thyroidectomy. It’s performed with incisions that can either be made high in the neck area or via the chest and armpit. This approach to surgery is performed in a way that avoids the need to make a cut in the center of the neck.
What Happens After Surgery?
Because a thyroidectomy is performed under general anesthesia, there is usually a need for a brief observation period after surgery. A drain may be temporarily placed in the neck so that excess fluid can safely exit the surgical site. There may be short-term hoarseness or throat soreness following the procedure. This may occur if a breathing (endotracheal) tube was used during surgery, or it may be the result of nerve irritation. Most patients are able to resume their normal activities shortly after having a partial or full thyroidectomy. However, strenuous activities should be avoided for a few weeks post-procedure.
If your entire thyroid gland has to be removed, you’ll need to take a pill every day. The medication prescribed is usually levothyroxine, a synthetic thyroid hormone also used to treat hypothyroidism (an underactive thyroid). You’ll need periodic blood tests so the appropriate approach to thyroid hormone replacement can be recommended. Thyroid removal is generally considered a safe procedure for most patients. With partial removal, the remaining part of the thyroid usually takes over the functions previously controlled by the entire gland.
